Radiofrequency is a low power, high frequency energy that causes a tiny region of the heart near the tip of the catheter to increase in temperature, thus ablating (or cauterising) a small area of abnormal tissue. Radiofrequency energy has been used for decades by surgeons to cut tissue or to stop bleeding. For the treatment of palpitations, a much lower power of radio-frequency energy is used.
You will be transferred to the Electrophysiology Laboratory (EP lab) from your ward. Usually before leaving your ward, you will be given a light sedative and your groin will be shaved.
The EP lab has a patient table, X-Ray tube, ECG monitors and various equipment. The staff in the lab will all be dressed in hospital theater clothes and during the procedure will be wearing hats and masks.
Many ECG monitoring electrodes will be attached to your chest area and patches to your chest and back. These patches may momentarily feel cool on your skin.
A nurse or doctor will insert an intravenous line, usually into the back of your hand. This is needed as a reliable way to give you medications during the study without further injections. You will also be given further sedation if and as required. You will also have a blood-pressure cuff attached to your arm that will automatically inflate at various times throughout the procedure.
The oxygen level of your blood will also be measured during the EP study and a small plastic device will be fitted on your finger for this purpose. Your groin area and possibly your neck will be washed with an antiseptic cleansing liquid and you will be covered with sterile sheets, leaving these areas exposed.
An anaesthetist will be present for many procedures. The procedure may be performed under local anaesthetic with sedative medication or under full general anaesthetic. This will be discussed with you before the procedure.
If the procedure is performed under local anaesthetic, the doctor will inject the anaesthetic to the area in the groin where the catheters are to be placed. After that, you may feel pressure as the doctor inserts the catheters but you should not feel pain. If there is any discomfort you should tell the nursing staff so that more local anaesthetic and sedative medication can be given. Occasionally it is also necessary to place a catheter in a vein in the side of the neck.
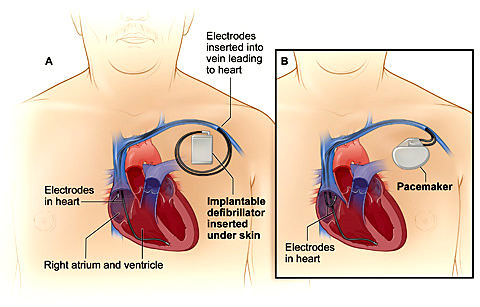
The catheters are positioned in your heart using X-Ray guidance. Once the catheters are in place you may feel your heart being stimulated and usually your abnormal heart rhythm will be induced. When the type of abnormal rhythm has been identified and the abnormal tissue localised, the radiofrequency ablation will be applied to this spot. This may cause a transient warm discomfort in the chest.
Radiofrequency ablation procedures are lengthy and the average duration is approximately 2 to 3 hours.