-Senior Consultant Cardiologist & Electrophysiologist
-Chief, Cardiac Pacing and Arrhythmia Services
-Department of Cardiac Pacing and Electrophysiology
-Apollo Hospitals, Greams Road, Chennai.
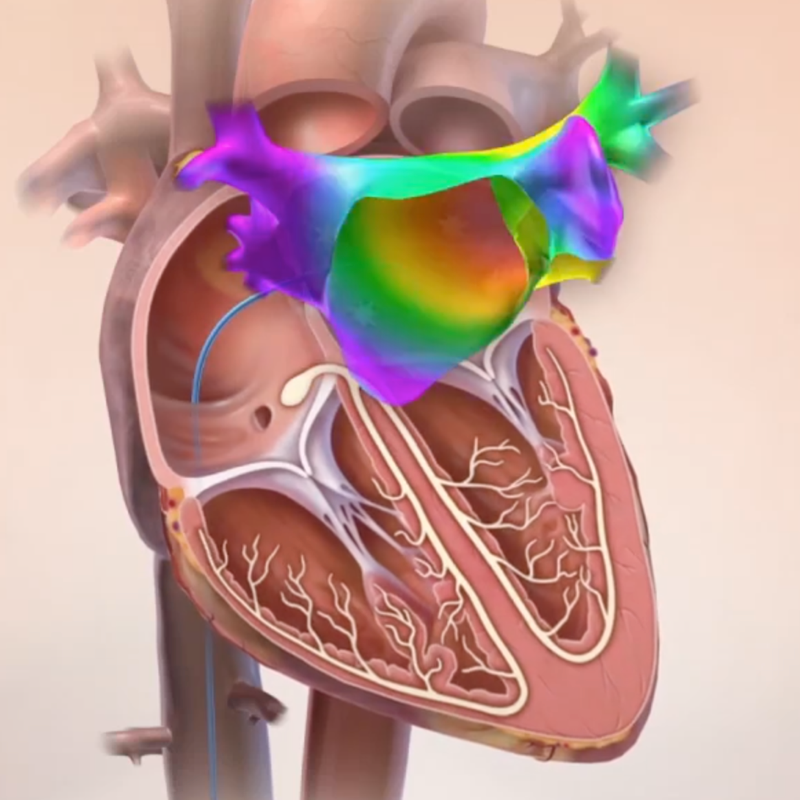
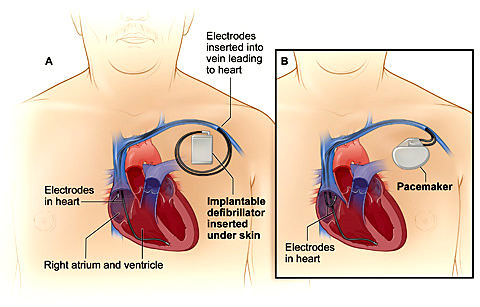
Some people with irregular heart rhythms (arrhythmias), medication alone may be enough to restore a normal heart rhythm. However, many patients with arrhythmias require more advanced treatment.
An electrophysiology study (EPS) is usually performed to diagnose the cause of the irregular heart rhythm. During the EP study or immediately after, an electrophysiologist may also perform a procedure to treat the arrhythmia.
Advanced treatment procedures include:

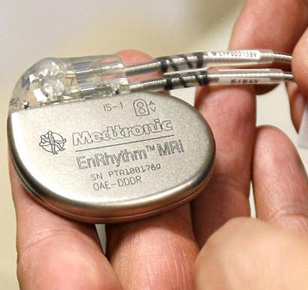
Using properly operating household appliances such as microwave ovens, electric blankets and most power tools cannot damage your pacemaker.
Using electric arc welders or working on automobile ignition systems will also not damage your pacemaker, however there is a possibility that they may interfere with the proper operation of your pacemaker. If you are using any of these or similar devices and become light headed or feel palpitations simply turn the device off or walk away from it and normal pacemaker operation should resume.
MEDICAL OR SURGICAL TREATMENT
If you are having any type of medical procedure performed, let your physician, dentist, chiropractor, physiotherapist or any health or cosmetic care provider know that you have a pacemaker. They will then be able to determine which diagnostic or therapeutic equipment is appropriate to use.
The following items do not affect the function of your pacemaker.
Acceptable:
The following items do affect the function of your pacemaker in close proximity.
You must not be too close to these appliances; more than 6 inches away
You must be at least 2 feet away from these appliances.
When using an induction range for cooking keep your pacemaker 2 feet from the range to prevent EMI.
Yes.
It is safe to use electric gardening tools. Included are the following tools:
MOTOR VEHICLE REPAIR
Acceptable with precautions
CONTRAINDICATIONS WITH PACEMAKERS
Not recommended:
Avoid using a power tool locked in the on position. This would prevent you from quickly turning off the equipment.
Avoid using a gas-powered chain saw. This is recommended because your hands and body come into close contact with the electric spark generating components/ these components could interact with your pacemaker.
Workplace Guidelines
After recovering from surgery most pacemaker patients can return to work or school. This section offers precautions and guidelines about using or working near various kinds of equipment or sources of high electrical current.
Office based employment.
Acceptable:
Most office equipment is safe to use with your pacemaker. This includes the following items and other similar equipment.
Travel and Security System Guidelines in Airports and Shops:
Most people with pacemakers can travel without taking special precautions. However certain security systems require a few instructions.
Acceptable
The following devices do not affect your pacemaker. However you may wish to know about these devices before you encounter them.
Acceptable with precaution
Other electrical devices. Do not stand close to any electrical device if you suspect it is causing a problem with your pacemaker.
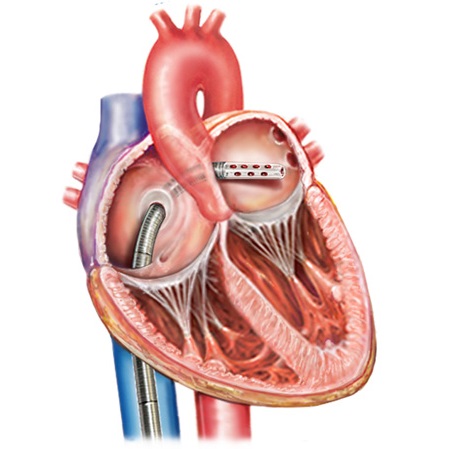
Quality of Care: Most Cardiac Arrhythmias can be treated and cured by Catheter Ablation thereby eliminating the need for life-long therapy.
Quality of Life: Catheter Ablation can restore the quality of life of the patient leading to a happier family life and improved productivity at workplace.
Save Lives: Some life-threatening Ventricular Arrhythmias can be successfully treated with Catheter Ablation there by providing patients with an option to live.
Cost of Care: The overall lifecycle costs of care for the patient may be reduced due the curative nature of Catheter Ablation therapy.
-Senior Consultant Cardiologist & Electrophysiologist
-Chief, Cardiac Pacing and Arrhythmia Services
-Department of Cardiac Pacing and Electrophysiology
-Apollo Hospitals, Greams Road, Chennai.